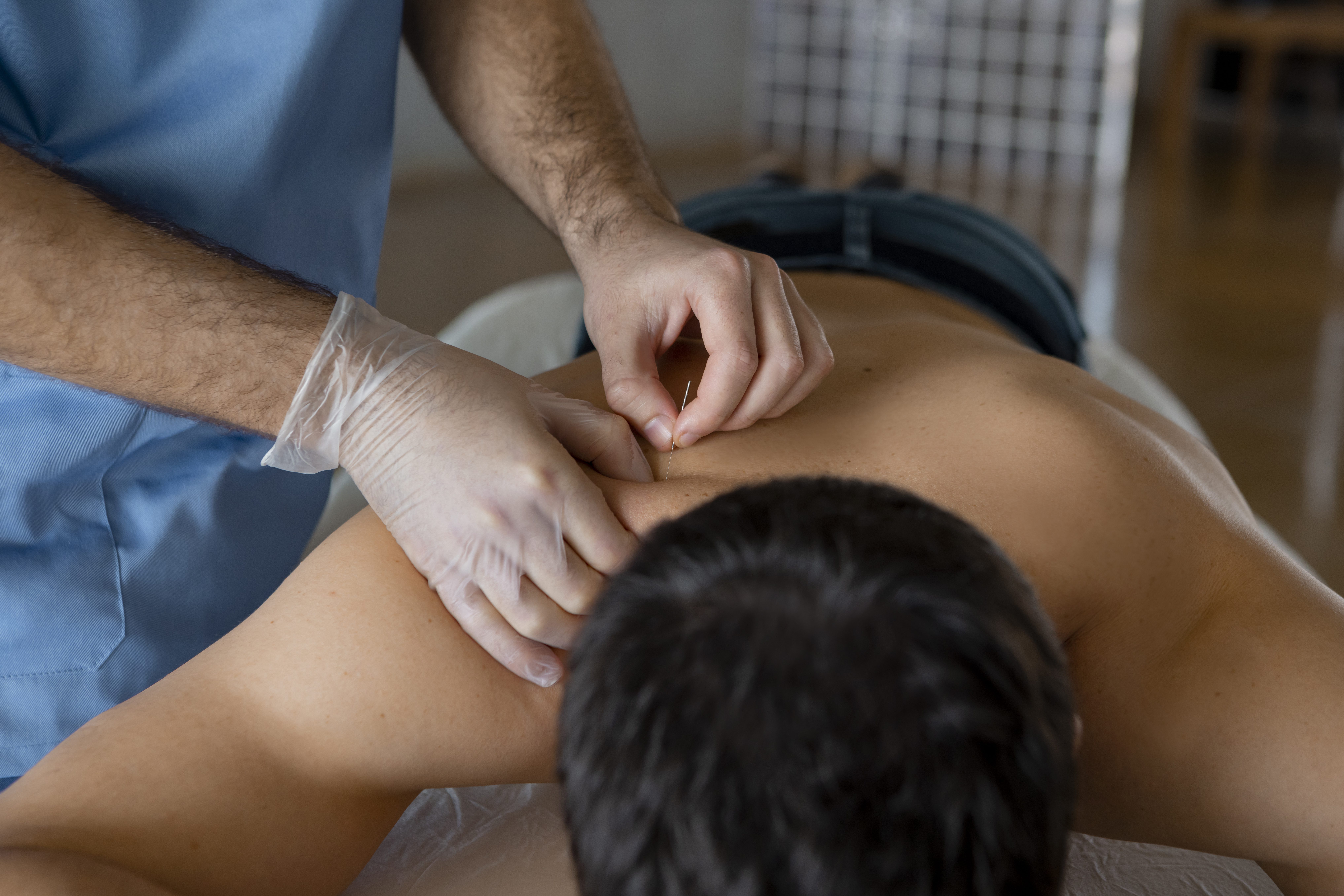
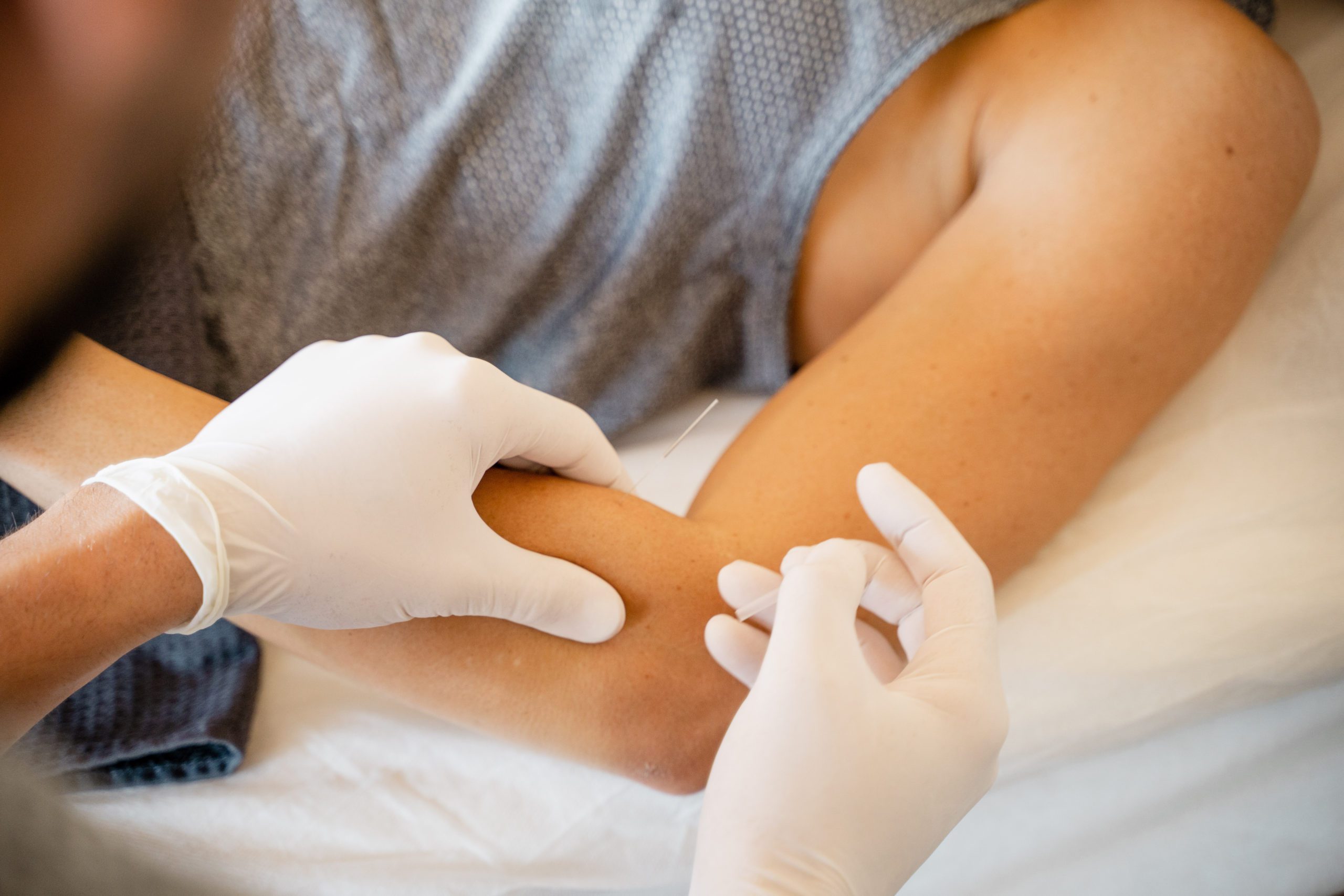
What is dry needling?
Dry needling is a physical therapy technique where the physical therapist uses very thin needles to penetrate skin and muscles, triggering a twitch response. This causes muscles to loosen and lengthen, which helps relieve pain. Some patients report feeling a slight pinch when the needles are inserted, but most describe the procedure as relatively painless.